Find a Doctor
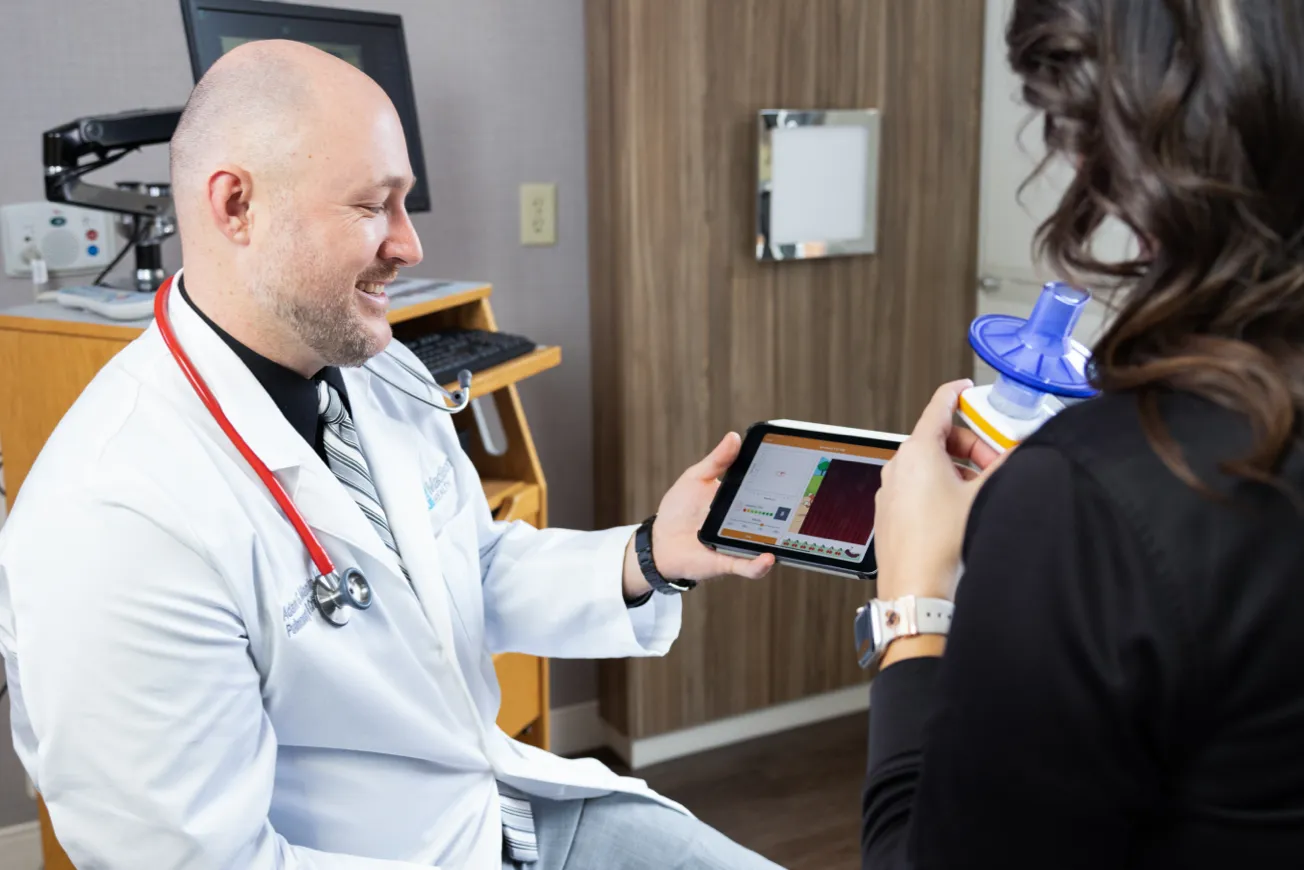
At Madison Health, you’ll find a provider to meet the needs of your entire family from experienced, compassionate primary care physicians to expert specialists.
My Madison Health
At Madison Health, we believe that every story matters. My Madison Health is more than just a campaign — it’s a reflection of the connections, care, and community that make us who we are. What does My Madison Health mean to you?

Join Our Team
Apply now to join the Madison Health team and experience our mission.


Supporting Our Vision
Through charitable gifts and fundraising activities, the Madison Health Foundation supports Madison Health and close-to-home healthcare services. We invite you to be part of this important mission.